Eswatini's Struggle with HIV and the Promise of Lenacapavir
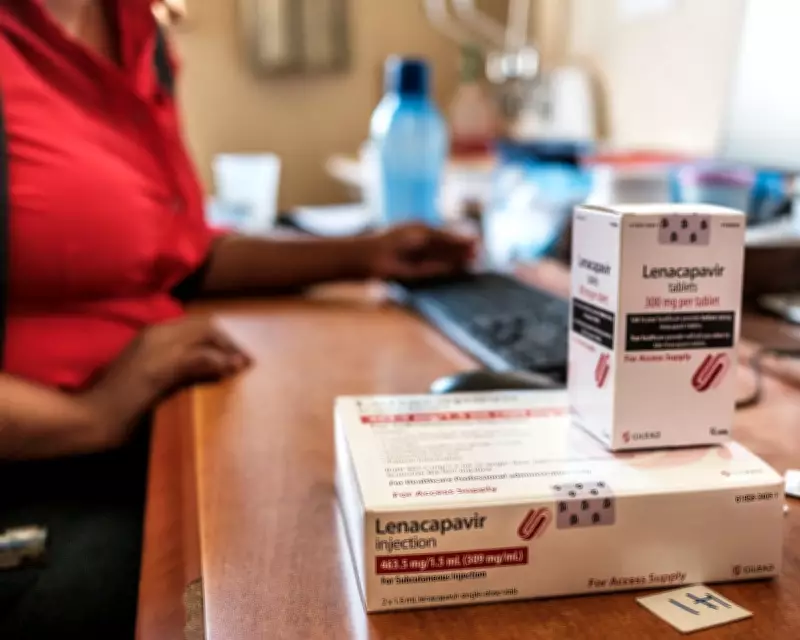
Eswatini, a southern African nation formerly known as Swaziland, holds the grim distinction of having the world's highest HIV prevalence, with approximately one in four people infected. Each year, about 4,000 new HIV infections occur among its population of 1.2 million. In response, the country has begun rolling out lenacapavir, a groundbreaking drug administered as an injection every six months to prevent HIV contraction. Often referred to as a "miracle" drug by patients and clinicians, lenacapavir offers hope in turning off the tap of new infections. However, its arrival in Eswatini is marred by significant supply shortages, raising questions about its effectiveness in combating the epidemic.
Limited Supply and High Demand
The amount of lenacapavir reaching Eswatini is described as "not even a drop in the ocean" by Dr. Nkululeko Dube, country programme director for the Aids Healthcare Foundation Eswatini. As of mid-March, only 2,995 people had started taking the drug, with coverage remaining extremely low despite high interest. The Global Fund to Fight HIV, Tuberculosis and Malaria is providing 6,000 doses in 2026, with 4,200 already delivered and the rest due in April. An additional US government-funded shipment is expected later this year. At clinics like Lobamba, doses are running out within days, highlighting the urgent need for more supply to reach all at-risk populations.
Targeting High-Risk Groups
Eswatini's strategy prioritizes key groups for lenacapavir access, including teenage girls and young women, who account for three-quarters of new infections, as well as pregnant and breastfeeding mothers, and sex workers. Sindy Matse, programme manager for the Eswatini National Aids Programme, emphasizes that anyone requesting lenacapavir should not be denied to avoid stigmatization. However, other high-risk groups, such as men who have sex with men, transgender women, people who inject drugs, and transport workers, face barriers in accessing care due to clinic attitudes and funding cuts, particularly from US aid reductions that have disrupted HIV prevention efforts.
Personal Stories of Struggle and Hope
Precious, a 32-year-old sex worker, exemplifies the challenges faced by many in Eswatini. Fleeing an abusive marriage, she turned to sex work to support her children, often facing financial incentives to forgo condom use. After testing negative for HIV, she received lenacapavir at the Lobamba clinic, including pills and injections, securing protection for six months. Similarly, Princess, a 27-year-old sex worker, sought the drug but was instead given post-exposure prophylaxis pills due to recent unprotected sex, underscoring the precarious access to lenacapavir. Both women's stories highlight the intersection of poverty, gender dynamics, and healthcare access in the fight against HIV.
Economic and Logistical Hurdles
Lenacapavir's cost presents another barrier. In the US, it costs $28,218 per patient annually, but through agreements with the Global Fund, poorer countries like Eswatini pay about $60 per person per year. Generic versions are expected to reduce this to $40 by 2027, potentially dropping to $25 with sufficient demand. However, manufacturer Gilead has faced criticism for restricting access to cheaper supplies and refusing direct sales to humanitarian organizations. Mduduzi Matsebula, Eswatini's health minister, remains optimistic, stating the government is prepared to fund lenacapavir domestically and aims to end AIDS as a public health threat by 2028, ahead of the global 2030 target.
The Path Forward
Despite the current limitations, lenacapavir represents a significant advancement in HIV prevention, being the first drug to reach sub-Saharan Africa in the same year as higher-income countries. Mark Edington of the Global Fund notes that while limited volumes may not drastically reduce infection rates this year, the drug could be a gamechanger by 2027-28 with generic availability. For Eswatini, success hinges on expanding supply, addressing stigma, and ensuring equitable access to all at-risk communities, as the nation strives to overcome one of the world's most severe HIV epidemics.








