Malawi's Polio Outbreak Sparks Massive Vaccination Drive Amid Global Eradication Struggles
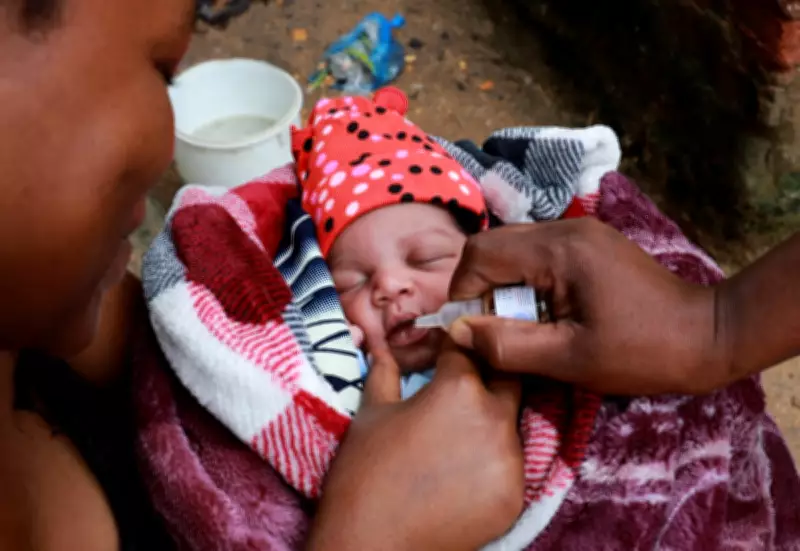
In Blantyre, Malawi, Mary Julius cradles her baby as the infant receives the first polio vaccine, marking the start of a critical national vaccination campaign. This effort comes in response to a new polio outbreak, the country's first in years, detected through environmental samples from sewage plants in Blantyre, Malawi's second-largest city. The outbreak has triggered an emergency response, with the World Health Organization airlifting supplies to support the drive.
Rapid Response and Vaccination Efforts
Within just four days, Malawi has vaccinated an astonishing 1.3 million children against polio, showcasing a swift mobilization in one of the world's poorest nations. This rapid action is crucial, as a single case of polio poses significant danger in areas with low vaccination rates. The virus is highly infectious, often spreading silently with mild symptoms, but it can lead to permanent paralysis or death, especially in children. Malawi had not recorded a wild poliovirus case since 2022, making this outbreak a stark setback.
The global fight to eradicate polio, which seemed within reach 28 years ago with only 2,880 cases in 20 countries, now faces renewed challenges. Dr. Jamal Ahmed, the WHO's polio chief, warns that eradication is an all-or-nothing endeavor, emphasizing the risk of resurgence if efforts falter. In Malawi, health workers are battling not just the virus but also community mistrust and misinformation.
Community Engagement and Vaccine Hesitancy
In Ndirande township, Blantyre, community health workers have visited nurseries, primary schools, and homes to administer vaccines. However, vaccine hesitancy remains a hurdle. Among young mothers aged 21 to 31, half were unaware of the disease, while others expressed reluctance. Frida Seva, a 21-year-old mother, stated, "My child is four years old but I don't know much about the vaccine. I am also not interested in getting the child vaccinated. I feel my child has had enough vaccines in her life."
At Chisime primary school, about one in ten children did not receive the vaccine due to parental refusal, often linked to religious beliefs or personal choice, as noted by teacher Georgina Donasi. To counter this, Malawi has mobilized social mobilizers, health workers, religious leaders, and traditional authorities to correct misinformation and build trust. Their efforts have shown success, with 45 out of 84 initially reluctant households in Ndirande accepting vaccination after targeted engagement.
Global Challenges and Misinformation
Similar struggles are evident in polio's remaining strongholds, such as Afghanistan and Pakistan, where the wild virus remains endemic. Sheeba Afghani, a senior manager with Unicef's polio eradication programme, highlights the power of local influencers in overcoming resistance. "You can give her any argument," Afghani says. "It doesn't matter. And then you have a local influencer walk in, and he says 'vaccinate', and she just hands you the child."
Misinformation, amplified by social media, poses a significant threat. Prof Heidi Larson, director of the Vaccine Confidence Project, notes that phrases like "vaccine-derived" can lead to innocent misunderstandings, suggesting vaccines cause polio, which is false. In the US, figures like Robert F Kennedy Jr have cast doubt on vaccinations, fueling confusion. Past incidents in Pakistan, where staged videos led to panic and violence, underscore the dangers of misinformation in vaccination campaigns.
Funding Cuts and Health Infrastructure
Malawi's outbreak is a variant poliovirus, or circulating vaccine-derived poliovirus, which emerges in areas with poor sanitation and low vaccination rates. Last year, 225 such cases were reported globally. The fight is further hampered by funding cuts, with the Global Polio Eradication Initiative facing a $1.7 billion shortfall. Donors like the US and Britain have reduced aid, impacting Malawi, where 55% of health expenditure relies on external funding.
Dr. Mike Chisema, Malawi's immunisation programme manager, emphasizes the need for coordinated responses to protect children and prevent future disabilities. "The funding space has really shrunk," he says, affecting services beyond emergencies. Despite challenges, Malawi continues testing and community outreach to control the outbreak at its source.
Hope and Continued Efforts
In Afghanistan, restrictions on women by the Taliban have hindered vaccination drives, with half of last year's wild polio cases occurring there. Unicef teams use microinfluencers and social media monitoring to combat misinformation, responding swiftly to spikes in false rumors. In Malawi, health workers like James Tungama perform educational plays in schools to teach children about polio.
Ruth Kutaombe, holding her eight-month-old boy at Malabada health centre, exemplifies pro-vaccination sentiment. "It will protect him from contracting the disease," she says, highlighting the importance of community trust. As Malawi pushes forward with its vaccination campaign, the global community watches, hoping to turn the tide in the long battle to eradicate polio once and for all.








