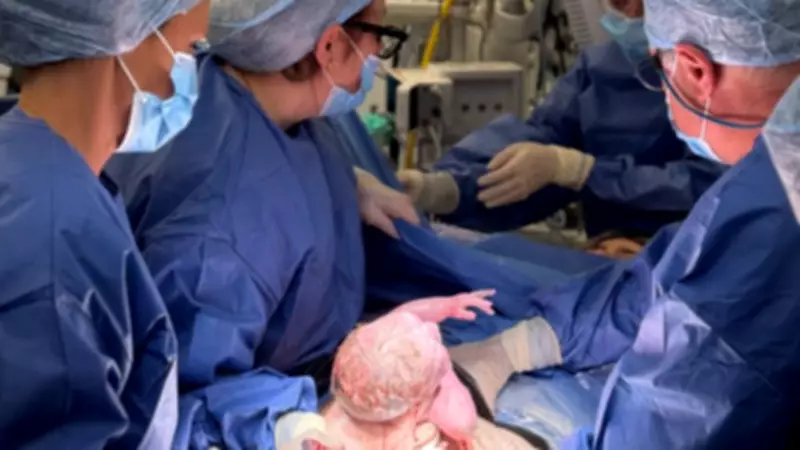
UK's First Baby Born from Deceased Donor Womb Transplant in London
A baby boy has made medical history as the first child in Britain born to a mother who received a womb transplant from a deceased donor. Hugo Powell was delivered by caesarean section in December at Queen Charlotte's and Chelsea Hospital in London, part of the Imperial College Healthcare NHS Trust, weighing 6lb 13oz (3.1kg). This landmark event marks only the third such case reported in Europe, following the UK's first birth from a living donor womb transplant last year.
A Mother's Miracle Journey
Hugo's mother, Grace Bell, an IT programme manager, was born with Mayer-Rokitansky-Kuster-Hauser (MRKH), a rare condition that results in an underdeveloped or missing womb. She described the birth as "simply a miracle" and expressed being the "happiest I've ever been in my life." Grace and her husband, Steve Powell, who works in finance, are both in their 30s and live in southern England. During the birth, Grace recalled holding Steve's hand and trying to peek over the curtain before Hugo was placed in her arms, a moment she found "quite unreal" after their long journey.
Steve Powell reflected on the overwhelming emotions, saying, "When he came over the curtain, it was just sort of overwhelming emotions. I felt like I wanted to cry, but couldn't." He emphasized that from their first meeting to having Hugo today, the experience has been "nothing short of a miracle after everything we've been through."
The Gift of Life and Donor Legacy
Grace Bell broke down in tears when recalling the moment she discovered she was pregnant, and she thinks of her womb donor daily. She hopes the donor's family "find some peace in knowing their daughter gave me the biggest gift, the gift of life." Expressing profound gratitude, she said, "There are no words to say thank you enough to my donor and her family. Their kindness and selflessness to a complete stranger is the reason I have been able to fulfil my lifelong dream of being a mum." Grace added that her child will always know about the incredible gift that brought him into the world.
The donor's parents shared their perspective, stating, "Losing our daughter has shattered our world in ways we can barely put into words. Yet even in this unimaginable pain, we've found a small measure of solace in knowing that her final act, her choice, was one of pure generosity." In addition to the womb, five other organs from the donor were transplanted into four people, saving multiple lives.
Overcoming Challenges and Pursuing Hope
After being diagnosed as a teenager with no womb, Grace Bell remembered "going into the hospital toilets and uncontrollably crying." She disclosed her condition to Steve Powell immediately when they met. Initially, the couple considered surrogacy before joining the womb transplant programme. Grace underwent a seven-hour womb transplant in 2024, followed by fertility treatment several months later. The couple may decide to have a second baby, after which surgeons will remove the transplanted womb to avoid long-term use of immunosuppressant drugs.
Key Facts About Womb Transplants in the UK
Donor Processes: For living donors, extensive counselling is required to ensure no coercion and understanding of risks. For deceased donors, the womb is not covered by normal organ donation consent; families must give specific permission after agreeing to donate other organs.
Shortage and Expansion: Womb Transplant UK runs programmes for both living and deceased donors. The living donor programme currently focuses on relatives, but may expand to friends or altruistic donors in the future. Transplants from deceased donors occur only with family consent.
Funding and NHS Role: Each womb transplant costs about £30,000, fully funded by the charity Womb Transplant UK, including NHS theatre time and ward stays. Operations are scheduled when NHS theatres are not in use, avoiding impact on waiting lists. Surgeons and staff volunteer their time. Once pregnant via self-funded IVF, patients receive NHS care like any other pregnancy.
Future Outlook: So far, five womb transplants have been performed in the UK—two from living donors and three from deceased donors, resulting in two births. Experts estimate up to 20-30 such transplants could be conducted annually in the future. Globally, about 25-30 babies have been born from deceased donor womb transplants.
Honoring Contributions and Emotional Moments
The couple gave Hugo the middle name Richard after Professor Richard Smith, clinical lead of Womb Transplant UK, and Norman after Grace's grandfather. Professor Smith, present at the birth, said holding Hugo and learning about the naming "brought a tear to my eye" and described it as "very emotional." This story highlights a significant advancement in reproductive medicine, offering hope to others with similar conditions.








